Health Care Chaplaincy Is Growing Field
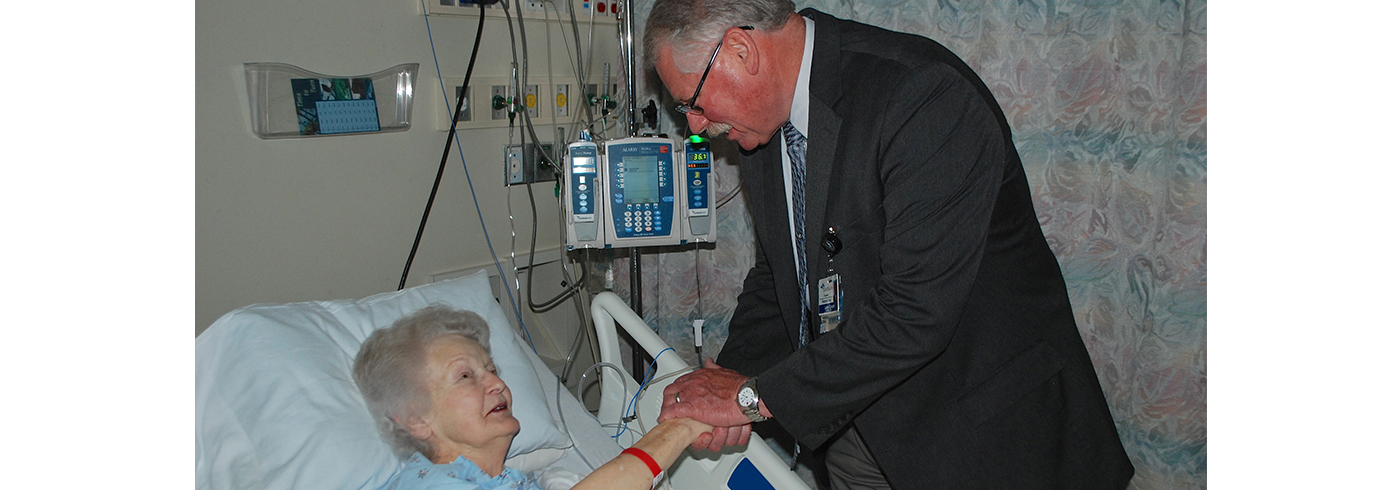
Larry D. Cooper serves as Assemblies of God Chaplaincy Ministries health care representative in a growing field in which he oversees 160 chaplains serving primarily in hospitals, hospice, palliative care centers, nursing homes, and long-term living facilities.
"I see this area mushrooming as time goes on," says Cooper, who has held the post since 2010. "As the population is aging and as people live longer, everybody needs health care."
Cooper, who also has been a hospital chaplain at Cox South in Springfield, Missouri, since 1986, says accrediting associations now recognize the value of the spiritual care that needs to be provided to patient families and medical staff.
"At the time when people are hurting the most they need a chaplain to come alongside to care for them," says Cooper, who succeeded Emanuel Williams, the first AG national health care representative. "If chaplains are able to be there at the initial time of grief, they can make a significant difference by setting people on a healing path toward recovery. If a chaplain can walk someone through their most difficult experiences, that person won't forget."
Health care chaplains have the unusual opportunity to minister to those along life's full spectrum, from newborns to centenarians. Cooper also notes that the population overall is attending church less, meaning contact with a health care chaplain may represent someone's only spiritual interaction during illness or before death.
"A chaplain may have the opportunity to see a person only once," Cooper says. "The chaplain must be able to initiate a relationship and try to meet needs by sharing God's love. For some people, it is their last opportunity to secure their eternal destination."
As one of seven full-time staff chaplains at the Cox medical complex, Cooper found a ministry niche providing pastoral care and support to patients, their families, and staff.
"Chaplains often have journeyed with patients and families over a lengthy period," Cooper says. "They give of their time, their hearts, and their energy. In some ways, a chaplain becomes a tangible expression of God's love."
Cooper obtained his master's of divinity degree from Assemblies of God Theological Seminary (AGTS) in 1979. He worked his way through seminary while an attendant at a funeral home, learning many facets of grief.
Patient hospital stays have grown shorter with the shift to outpatient surgeries and that means there is more of a role for laypeople ministering to the needs of those who have had operations, Cooper says.
"The Church will need to be more assertive in reaching out to care for those in the congregation as they recover," Cooper says.
Cooper has a history of creating methods to meet needs. While serving as pastor of New Life Assembly of God in Albion, Nebraska, Cooper developed a weekly Bible study at a local nursing home. Due to overwhelming participation from staff and residents, including those in an adjacent assisted-living facility, the administrator asked Cooper to become chaplain at the nursing home in 1983. This prepared him for his eventual longtime vocation of full-time chaplain.
Colleagues at Cox South commend Cooper for going beyond the normal call of duty. For instance, Cooper coordinates pastoral care volunteers, supervises practicum students, conducts in-service training for staff in areas ranging from postmortem care to organ/tissue donation, and serves on multiple planning committees.
In 2000, Cooper co-founded the Critical Incident Stress Management (CISM) team at Cox South. He served 12 years as clinical coordinator, then program coordinator. He continues in a mentoring role to program leaders.
Longtime co-worker David Hoover, a paramedic and educator at Cox, calls Cooper an innovator because of his ability to care for employees as much as patients.
"Larry always has been a good influence on the staff, making sure they know they are cared for, not just by him but by the programs he has helped put into place," Hoover says. "By helping to implement the CISM program, he recognized how caregivers get stressed with the patients they care for, and he put in protections for them."
Susan Crum, program director for the flight program at Cox Hospitals, likewise notes that Cooper seems to always be available in a crisis, even with the duties he has added to his portfolio. She says Cooper is able to provide counsel and comfort to flight nurses and paramedics who have witnessed traumatic episodes while treating injured patients.
"He obviously visits with patients and their families and is there for their needs," Crum says. "But he also is there for the emergency department staff and personal needs, sitting with us, crying with us."
In addition to all his other responsibilities, Cooper is an AGTS adjunct professor teaching hospital ministries. He obtained a doctorate of ministry in 2004 from the seminary by writing a dissertation on managing conflict situations by understanding and responding to difficult families.
 ASSEMBLIES OF GOD
ASSEMBLIES OF GOD